“When my husband and I went to our fertility specialist and she told us that we would be good candidates for IVF, we started on the typical journey,” remembers author Nadine Kenney Johnstone. But her experience would be far from typical.
In 2012, the then 28-year-old sought infertility treatment after trying naturally for almost a year. She and her husband Jamie were living in the suburbs of Massachusetts, where he worked as a chef and she taught English at Framingham State University.
While many women who pursue IVF are well into their thirties, the young couple had extenuating circumstances. Jamie was a testicular cancer survivor, and an analysis had revealed that the chemotherapy treatments had compromised his sperm motility. At the same time, Johnstone, who had recently stopped taking birth control, discovered she wasn’t ovulating.
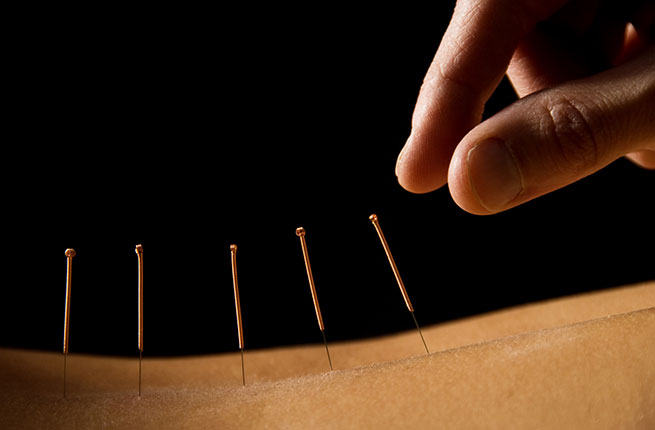
Johnstone began with the egg retrieval procedure, a standard precursor to IVF in which the woman receives hormonal injections that stimulate her ovaries to release extra egg follicles, which are then harvested and inseminated with sperm in a petri dish.
But when she got home from the procedure, she felt dizzy and nauseous, with sharp pains in her abdomen. She started crying and throwing up.
Her husband rushed her to the ER, where an ultrasound of her abdomen revealed that she was bleeding internally. She went into emergency surgery.
“Unbeknownst to me, my left ovary never clotted after the retrieval,” she explains. The surgeons sutured her ovary, and after a few days, she left the hospital with a six inch scar, from her belly button down to her pubic bone, and began a painful, prolonged recovery.
According to fertility expert Dr. Brooke Hodes-Wertz of NYU Langone, what happened to Johnstone is extremely rare. “The egg retrieval procedure is minimally invasive and there’s less than a one percent chance of bleeding and infection,” she tells us. What’s more common is ovarian hyperstimulation syndrome, a condition which can occur due to an oversaturation of hormones, and can cause abdominal pain, nausea, and in severe cases, blood clots and kidney failure.
The egg retrieval setback was only the beginning of Johnstone’s troubles. While the typical next step of IVF would be to implant the fertilized embryo into her uterus, Johnstone was still very much physically — and mentally — recovering. Instead, they froze the embryos and waited six months to try again.
Six months later, things still didn’t go as planned.
“In order to prepare your body for the transfer, you have to take estrogen,” Johnstone explains. But that gave her constant headaches, and even impaired the vision in her left eye. “We had to cancel that cycle.”
Three months later, Johnstone tried again and was able to successfully transfer a couple embryos. “But either my body rejected them, or they rejected me, and I didn’t become pregnant from it,” she says. (IVF varies from person to person. While some women become pregnant after the first cycle, it’s not uncommon for others to require multiple cycles before conceiving.)
That August, Johnstone and her husband made what would be their final appointment with a fertility specialist. “I was just so done with IVF,” Johnstone remembers. “I asked the doctor, ‘What else can we do?’ And he just shook his head.”
It turns out she was pregnant while sitting in his office, but she didn’t know it. She had conceived naturally at the age of 29.
Johnstone has detailed the harrowing, but ultimately hopeful experience in her memoir, “Of This Much I’m Sure,” out this month on She Writes Press. The now 33-year-old lives in Chicago with her family, where she teaches English at Loyola University and Jamie works as a project manager at a corporate signage company. Their son Geo is now four years old.
At this point, she and Jamie are uncertain whether they’ll have more kids. “I know I would never try IVF again,” she says. “I can’t go down that road again, for my own sanity.”
Johnstone’s biggest takeaway from the experience: realizing how important it was “to reach out and share our pain with other people and ask for comfort.”
“When I was at the lowest point, I got an email from my husband’s cousin Amy. She’s a life coach and a doula. Her first sentences were: ‘You will have a baby, of this much I am sure,’” she recalls, citing the line that inspired her book’s title.
“I cannot tell you how hopeful and uplifting it was just to hear someone speak in affirmative, confident language,” she says. “It gave us the hope and endurance we needed to keep going. So, speak. Speak to yourself, to other people. But whatever you do, do not keep this journey a secret.”