ZURICH (Reuters) – Many studies assessing the accuracy of COVID-19 antibody tests had major shortcomings, a review released on Thursday concluded, offering further evidence the blood tests are of little use for people seeking to know with certainty if they have been infected.
Cochrane, a British-based journal that reviews research evidence to help decision makers adopt better health policies, looked at 54 studies, mostly from Asia, that sought to measure the reliability of tests purporting to show whether somebody has developed antibodies against the new coronavirus.
The studies were often small, did not use the most reliable methods, and results were often incomplete, Cochrane said in its 310-page report.
Also, most of those tested had been admitted to hospital, offering no insight into how well the tests could detect antibodies in the majority of people with milder symptoms.
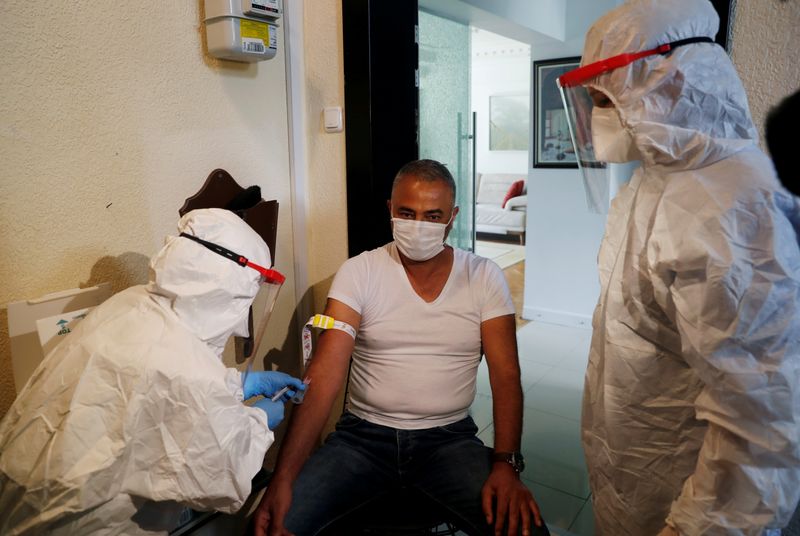
There is intense interest in these antibody tests, which rely on either a finger prick or a venous blood draw, by people eager to know whether they have had COVID-19 or not.
There has been speculation that a positive result might mean people have some protection, at least temporarily, against re-infection. Such hopes are unrealistic, said Jon Deeks, a professor of biostatistics at the University of Birmingham who leads Cochrane’s test evaluation efforts.
“A lot of people in the UK are very interested and keen to know, but there is no decision they should be making at the moment based on the results of that test,” Deeks told reporters.
In all, the Cochrane researchers identified data from 25 commercial COVID-19 tests, a fraction of roughly 300 such tests that exist. Their review did not include tests offered by Roche or Abbott Laboratories, which were approved by regulators after the cut-off deadline of April 27.
Updates of Cochrane’s report plan to include data from both companies’ tests, which are now being sold by the millions in the United States and Europe.
While the studies reviewed by Cochrane showed the antibody tests were better at detecting COVID-19 antibodies in people two or more weeks after their symptoms started, they did not provide clues as to how well they work in patients further from infection.
Such gaps undermine the value of tests as tools in so-called “seroprevalence studies”, to determine what percentage of people in a population may have been exposed to the virus.
“We don’t know how well these tests work beyond five weeks, so that’s our greatest concern,” Deeks said. “In seroprevalence studies, you’re looking beyond that and really we need some data which says, ‘How well do they work at three months, four months, five months.'”
UNDER SCRUTINY
Scientific studies’ veracity has been under scrutiny during the pandemic, more so after British medical journal The Lancet issued an apology after publishing a study on health risks from the malaria drug hydroxychloroquine in COVID-19 patients that was retracted by three of its authors.
Cochrane said that of the 54 studies it looked at that covered nearly 16,000 samples, 89% had a high risk of bias based on how participants were selected, since they were unlikely to match patient populations in clinical practice.
There were more problems, Cochrane said, including often no mention of whether the samples were anonymized or blinded, potentially leading technicians to repeat tests if they thought they had got the wrong result.
Some studies withheld results, while others included five or more samples per patient, resulting in inflated sample sizes and results that were falsely precise, Deeks said.
“For many of the studies, we could never find out how many patients were included in them,” he said. “All we know is how many samples were tested.”
(Reporting by John Miller, Editing by Timothy Heritage)