(Reuters) – The following is a roundup of some of the latest scientific studies on the novel coronavirus and efforts to find treatments and vaccines for COVID-19, the illness caused by the virus.
Viral load predicts need for ventilator, death risk
When COVID-19 patients are admitted to the hospital because of pneumonia, doctors can estimate their risk of needing mechanical breathing support or dying based on their “viral load” – the amount of virus genetic material obtained by swabbing the back of the nose and throat, a new study suggests. “This risk can be predicted regardless of how sick they are when they are admitted, what other comorbidities they may have, their age or how many days they had symptoms,” coauthor Dr. Ioannis Zacharioudakis of NYU School of Medicine told Reuters. His team studied 314 patients, dividing them into three groups according to viral load upon hospital admission. The group with highest viral levels had 59% higher odds of becoming critically ill or dying than the lowest viral load group. The data, published on Friday in Annals of the American Thoracic Society, “will have practical implications in our ability to judge which patients will benefit the most from early escalation of care, treatment with antivirals and/or inclusion in trials of new therapeutics,” Zacharioudakis said. (https://bit.ly/3oJijtQ)
Coronavirus damages red blood cell membranes
The new coronavirus damages the membranes of oxygen-carrying red blood cells, contributing to the hypoxemia, or low blood concentrations of oxygen, common in COVID-19, researchers have found. Signs of hypoxemia can range from shortness of breath to organ and tissue damage. Studying blood samples from COVID-19 patients and healthy individuals, researchers found the virus did not appear to affect red cells’ ability to pick up oxygen and deliver it throughout the body. But patients had “clear damage” to red cell membranes, in particular to a membrane protein responsible for helping the cell survive injuries. As a result, patients’ red cells might be more vulnerable to so-called oxidative stress and other injury, coauthor Angelo D’Alessandro of the University of Colorado Denver said in an email. Red cells circulate for up to 120 days before the body replaces them with new ones, and they cannot synthesize new components to replace the damaged parts. This might help explain why some COVID-19 symptoms can last for months, D’Alessandro said. (https://bit.ly/3mMBq4A)
Pandemic exacts toll on ER doctors’ mental health
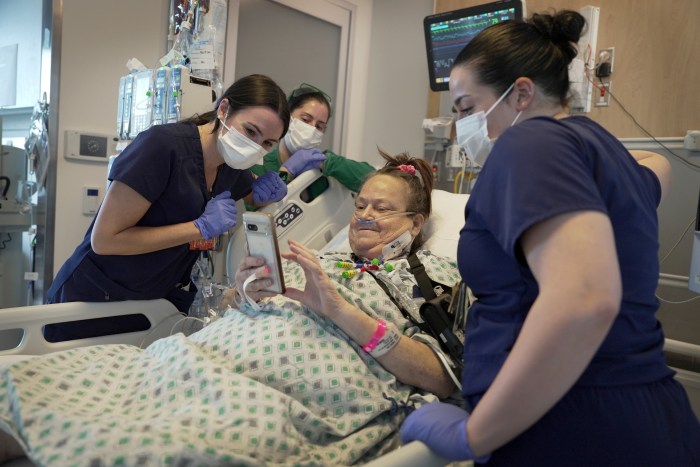
COVID-19 is taking a toll on emergency physicians’ mental health and many are reluctant to seek help, according to poll results reported at the American College of Emergency Physicians (ACEP) annual meeting. Among a nationally representative group of 862 U.S. emergency physicians, 87% reported feeling more stressed since the pandemic began and 72% reported more burnout. More than 80% cited concern for their own health and safety, and the safety of their family and friends, around contracting COVID-19. Nearly half said they are uncomfortable seeking mental health services, 73% said there was at least some stigma to seeking these services in their workplace, and 57% said they would be concerned about their job if they sought mental health treatment. In April, New York City emergency physician Dr. Lorna Breen died by suicide while recovering from COVID-19. “With patients overflowing in the hallways, not enough personal protective equipment … and minimal supplies, my sister rose to meet the challenges of COVID-19,” Jennifer Breen Feist said at an ACEP news briefing. When Breen finally sought mental health treatment, her main concern was how she would be perceived at work, her sister added. (https://bit.ly/3e9rFdJ)
Heart failure history adds to risks for COVID-19 patients
A new study helps quantify the extra risks faced by people with heart failure and coronavirus infections severe enough to require hospitalization. Doctors at the Mount Sinai Health System in New York City studied 6,439 hospitalized COVID-19 patients, including 422 with a history of at least one heart failure episode. Compared to the other patients, those with a history of heart failure had longer average hospital stays (8 days vs 6 days), the doctors reported on Wednesday in the Journal of the American College of Cardiology. After accounting for other risk factors, the heart failure patients were more than three times more likely to need mechanical ventilation and nearly twice as likely to die. If future studies show similar patterns, the researchers conclude, doctors might need to consider using more aggressive therapies in patients with COVID-19 and a history of heart failure. (https://bit.ly/2TG2d5U)
Open https://tmsnrt.rs/3a5EyDh in an external browser for a Reuters graphic on vaccines and treatments in development.
(Reporting by Nancy Lapid and Megan Brooks; Editing by Bill Berkrot)