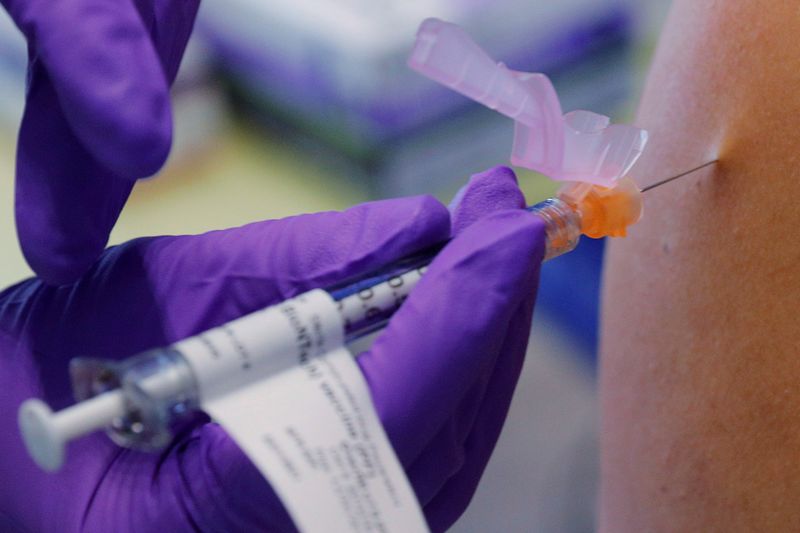
LOS ANGELES (Reuters) – From the wide-open spaces of a U.S. tribal nation to urban hospital emergency rooms, doctors, nurses and delivery people are wrestling with challenges in the roll-out of Pfizer and BioNTech’s COVID-19 vaccine – including delays, anxiety and keeping the drug at just the right level of cold.
U.S. Public Health Service Lieutenant Commander Erica Harker on Monday delivered a red, portable cooler with 165 doses of the vaccine to a hospital in tiny Ganado, Arizona, one of three drop-offs on a roughly 200-mile (322 km) round trip through the Navajo Nation, accompanied by tribal police.
The long-awaited vaccine – which must be stored at minus 70 degrees Celsius (minus 94°F) – comes in pizza-sized plastic boxes containing 975 doses, too much for many rural areas. When pharmacists like Harker crack open those boxes to extract vials, they start a 120-hour countdown to get the vaccine into arms.
“It wasn’t anything where we could just lollygag and take our time,” said Harker, who used a sensor to be sure that her deliveries stayed in a temperature range similar to that of a home refrigerator.
Big delivery companies experienced problems when a handful of trays bound for California and Alabama in Pfizer’s dry-ice cooled containers hit minus 92 Celsius (minus 197.6°F) in transit, which was too cold, U.S. Army General Gustave Perna said on a conference call on Wednesday.
“We locked those trays down … they never left the truck,” Perna said of those shipments.
WAITING ON PINS AND NEEDLES
Reserving initial doses for healthcare professionals made the roll-out somewhat easier.
“They are anxious to get the vaccine. Out of hundreds of clinical caregivers in round 1, only a handful have declined,” for reasonable issues such as pregnancy, said Marcy Brown, chief operating officer of Southern California’s Hoag Health Network, which experienced a vaccine delivery delay.
Oschner Health in Louisiana on Monday got about a tenth of the doses it prepared for at its New Orleans hospital – forcing staffers there to reschedule appointments.
“The biggest disappointment was expecting 9,500 doses … and getting much less,” said Dr. Sandra Kemmerly, the system medical director of hospital quality.
Despite the headaches that come with the nation’s largest and most complex vaccination campaign in history – healthcare workers said the release of the vaccine was a ray of hope after months of witnessing the deaths of patients and co-workers.
It is particularly poignant for workers in heavily hit areas, like the Navajo Nation.
The impact of the pandemic “is a memory that will be ingrained in our hearts, our mind and our souls, for a lifetime,” Harker, of the Public Health Service, said.
(Reporting by Lisa Baertlein and Deena Beasley in Los Angeles; editing by Peter Henderson and Stephen Coates)