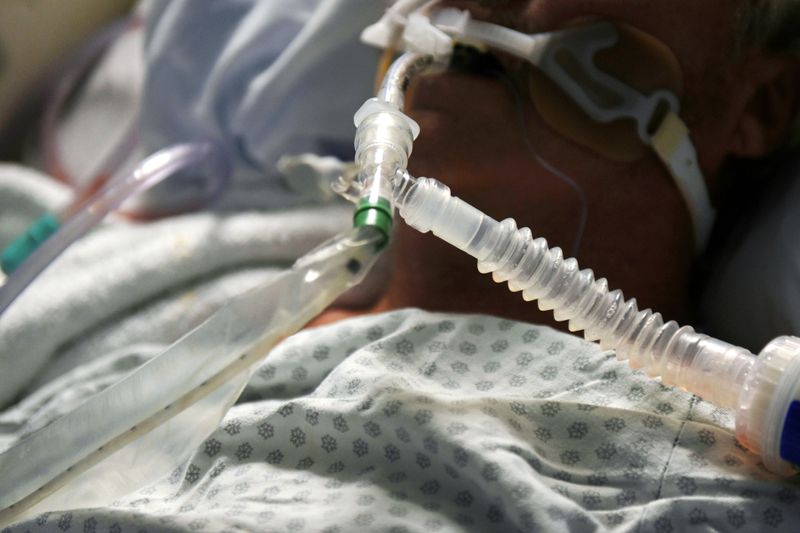
(Reuters) – With the COVID-19 pandemic sweeping across its shores earlier this year, the U.S. government in April announced orders for almost $3 billion of ventilators for a national stockpile, meant to save Americans suffering from severe respiratory problems brought on by the disease.
But of the 140,000 machines added since then by the government to the U.S. Strategic National Stockpile, almost half were basic breathing devices that don’t meet what medical specialists say are the minimum requirements for ventilators needed to treat Acute Respiratory Distress Syndrome, the main cause of death among COVID-19 patients, according to a Reuters review of publicly-available device specifications and interviews with doctors and industry executives.
Only about 10% are full intensive care unit (ICU) ventilators of a type that doctors and ventilator specialists say they would normally use to intubate patients suffering from Acute Respiratory Distress Syndrome or ARDS, the Reuters review found. The remainder – or about 40% – are transport ventilators normally employed for shorter periods but are considered sophisticated enough to be used long enough for ARDS patients to recover.
A September study by 22 ventilator specialists published in the official journal of the American College of Chest Physicians found half the models added to the stockpile were not suitable for treating ARDS.
The Reuters analysis is the first to examine the numbers of machines and their ability to save lives, according to those familiar with their use and published standards, and to tally the purchase cost to American taxpayers. The analysis is based on publicly-disclosed order details along with peer-reviewed studies about what types of ventilators are suitable for treating ARDS, interviews with medical specialists and World Health Organization guidance.
Many of the machines don’t meet the requirements of ARDS patients and their presence in the stockpile gives “a false sense of security,” Sajid Manzoor, director of adult respiratory therapy at The Johns Hopkins Hospital in Baltimore. “The COVID patients are so sick when they have ARDS. For the patients’ benefit we really need to stick with the full ICU ventilators,” he said.
A spokeswoman for the Department of Health and Human Services (HHS), which is responsible for making purchases for the national stockpile, said that an interagency task force on ventilators made recommendations on which models and quantities to procure in March, a time of “extreme projections for respiratory care needs.”
With little known about COVID-19 at the time, the HHS “was preparing for the worst possible scenario,” the spokeswoman said. HHS declined to share the medical advice it relied upon in setting its minimum requirements or in selecting devices.
She added that the federal government has since adjusted its response as more clinical data has become available about the treatment of COVID-19. For instance, she said, the HHS is now procuring kits to provide alternatives to intubation, such as plastic tubes that deliver oxygen into the nose.
Today, the United States is engulfed in a deadly escalation of the virus with more than 1.1 million new infections last week. The country has reported more than 268,000 coronavirus-related deaths in total since the pandemic began.
There is currently no ventilator supply crisis in the United States as other treatments, including steroids, have reduced the need for intubation. HHS and manufacturers of the more basic devices said they can have a role in dealing with less acute cases of COVID.
But three respiratory specialists with ICU experience, and who have published papers on ventilator use, told Reuters that the government should have only added machines that could be used for dealing with ARDS. With limited resources, they said, the focus in the spring should have solely been on machines that could save the most critically ill — and it was those types of machines that were in short supply at the time.
In a situation where the vast majority of patients in intensive care have serious respiratory issues, “you need complex ventilators to be able to support them,” said Dr Michael Christian, a London-based doctor who specializes in critical care medicine and an author of the September study.
The U.S. Strategic National Stockpile, the country’s largest store of medical supplies for use in a crisis, is intended to provide life-saving equipment in emergencies.
Respiratory care specialists – including HHS staff – have over the past decade said in congressional hearings and studies that the national stockpile should contain devices to help patients suffering from respiratory failure in the event of a flu-type pandemic.
Unlike full ICU ventilators, breathing devices that are designed as transport machines are meant to be used for short periods – typically hours – such as for getting critically-ill patients to ICU or treating non-critical breathing issues, rather than the weeks that COVID-19 patients can spend on a machine. As a result, the more basic versions frequently lack the lung-protecting features that would allow them to be used for more than hours, and experts say they have little chance of saving the lives of critically ill COVID-19 patients.
“MAY NOT HAVE BEEN IDEAL”
As COVID-19 swept through China and Europe early in the year, governments around the world scrambled to procure ventilators, mechanical devices that push carefully calibrated volumes of air and oxygen into the lungs via a tube in the windpipe. They are crucial for the care of people with respiratory failure, which is the primary killer of patients with COVID-19, the disease coronavirus causes.
In February, HHS Secretary Alex Azar said the U.S. stock of ventilators would not be sufficient to tackle a pandemic. Prior to the pandemic, the stockpile held some 14,000 machines, mostly sophisticated transport ventilators capable of dealing with severe respiratory distress.
In late March, President Donald Trump vowed the United States would make or otherwise procure 100,000 additional ventilators. Over the following weeks, the HHS announced a flurry of orders.
The HHS spokeswoman said there was a deliberate move to diversify the types of devices held in the stockpile to also include models designed for use in transport or temporary field hospitals in addition to those that meet requirements for use in ICUs.
“In the event that the infection curve could not be flattened, HHS was identifying and recommending procurement of as many respiratory care devices as available to meet the needs of healthcare facilities, even if those devices may not have been ideal,” she said.
Of the roughly 140,000 machines the stockpile had received by October, about 15,000 were ventilators that are specifically designed for use in intensive care units. Those machines cost on average about $21,600, according to HHS contract notices.
It also received some 58,000 machines that were designed for use while transporting critical patients to an ICU or within health facilities but also have some complex features such as pressure controls and the ability to vary oxygen levels that, according to medical specialists, could help COVID-19 patients suffering severe respiratory distress for days or potentially even weeks while they recover. The average cost of those kinds of machines added to the stockpile was about $16,800.
The government also spent about $450 million on roughly 66,000 units spanning four models that are designed for transporting critically ill patients for short periods and for providing care to patients with less acute respiratory problems. These devices, which are unlikely to save the lives of critically-ill COVID-19 patients, cost on average about $7,900 each.
None of the four models meet the minimum requirements for functionality for treating severely affected COVID-19 patients as identified by the World Health Organization (WHO) in guidance published in March, the Reuters analysis found.
Combat Medical, the maker of one of the models, said its device could help less acute COVID-19 patients. Manufacturers of the two other devices, Hill-Rom Holdings Inc’s and ResMed Inc, acknowledged that their devices did not meet all the WHO standards and also that their devices could help less acute COVID-19 patients.
“PUTS THE PATIENTS AT RISK”
A fourth model, made by a partnership between General Electric Co and Ford Motor Co., was the pNeuton. According to its specifications and experts familiar with the device, the pNeuton is not suitable for intubating severe COVID-19 patients with ARDS over a long period of time.
When California in July asked for 500 ventilators from the national stockpile, it received the pNeuton. But California, according to the state’s department of public health, needed more full-featured ventilators, prompting it to go back to the national stockpile. HHS then sent 500 ICU ventilators to the state, allowing California to also keep the pNeutons, both parties said.
Ford referred questions about the machine’s capabilities to General Electric, which declined to comment on whether it was suitable for treating COVID-19 patients with ARDS. According to a user manual for the pNeuton, it “has been specifically designed for patient support during transport and non-critical care unit mechanical ventilation.”
Richard Branson, a professor at the University of Cincinnati who has advised officials overseeing the national stockpile, said sending pNeutons when hospitals need ventilators that are suitable for intubating COVID-19 patients could have consequences.
“It’s a risk because if they get something they are not expecting and it isn’t capable of meeting the patients’ needs, then that puts the patients at risk,” he said. Without the right equipment at the right time, Branson said, “the patient won’t survive.”
(Reporting by Tom Bergin; Editing by Tom Lasseter and Cassell Bryan-Low)