President Trump is coming for your free birth control.
At least it seems that way. According to the Wall Street Journal, the president is finalizing plans to pull back an Obamacare rule that requires employers to provide free contraception in its company insurance plans. New requirements will allow employers to skip it if they object morally or religiously.
“The data suggest that Trump’s new rule could open up the floodgates for nearly anyone to force women to either pay out of pocket or navigate hurdles to obtaining additional coverage for contraception,” Jamila Taylor, senior fellow at CAP, said in a press release. “President Donald Trump and [HHS] Secretary Tom Price are, in effect, saying to women that any employer’s personal views can decide whether or not you get birth control.”
While you may not be able to control the government, you can control what happens to your body before the requirement goes into effect. One way to do that? Opt for long-term birth control in the form of an IUD.
What is an IUD?
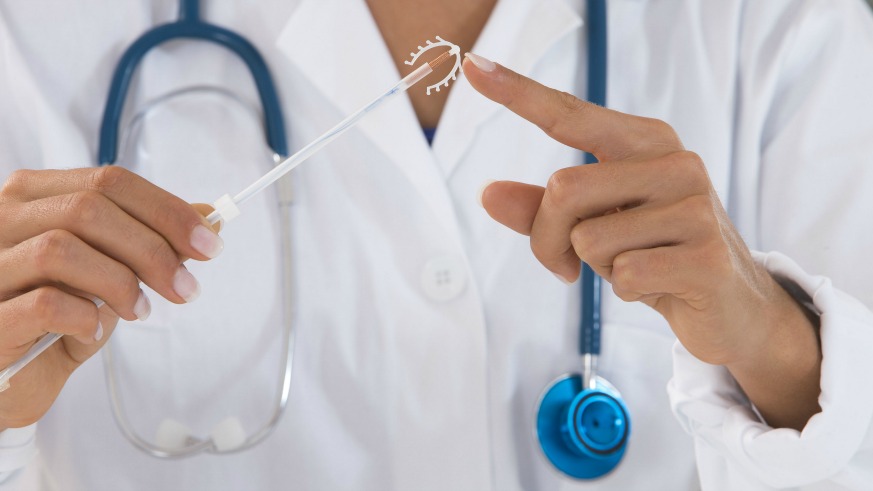
An IUD — short for intrauterine device — is a small t-shaped piece of plastic that’s inserted into the uterus for long-term birth control, up to 12 years in some cases.
IUD types
There are five FDA-approved IUDs currently on the market in the United States. Hormonal IUDs — Mirena, Skyla, Liletta and Kyleena — make up the majority of approved brands and work by releasing hormones into your body to help you ovulate less often and block sperm from attaching to an egg.
Skyla and Mirena are the stronger hormonal IUDs, but release hormones into the body at different intervals. Mirena contains 52 mg of levonorgestrel and releases 20 mcg into the body daily after insertion, eventually dropping to 10 mcg a day. Skyla, on the other hand, contains 13.5 mg of levonorgestrel and releases 20 mcg for the first so days after insertion before dropping to 5 mcg a day until it’s removed.
Both are designed for long-term use: Skyla IUDs last for three years, while Mirena IUDs are good for six years.
Two newer brands of hormonal IUDs, Liletta and Kyleena, also release levonorgestrel and are made to last for five and six years, respectively.
Copper IUDs (brand name: ParaGard) are good for up to 12 years and don’t contain hormones at all, but work by inducing inflammation in the uterus (via 176 mg of copper wire). This inflammation works against sperm, preventing it from attaching to an egg — or preventing a fertilized egg from attaching to the uterine wall.
IUD insertion
IUDs must be placed by a doctor and typically only takes about 15 minutes. To insert an IUD, a doctor has to push it past the cervix and into the uterus.
IUD pain
The downside to IUDs? They can be painful — women often report cramping both during and after an IUD is placed.
Choosing the right IUD depends on a number of factors, including health and the length of time birth control is needed. Hormonal IUDs can cause side effects like acne, breast tenderness, nausea and depression, while some women experience painful periods for six months after getting the copper IUD.
Size can also be a consideration: The Skyla and Kyleena IUDs are smaller than the rest, making them less painful for some women.
Though rare, the IUD can be expelled from the body in the weeks and months following insertion, especially during periods.
IUD effectiveness
IUDs are one of the most effective forms of birth control at 99 percent. Copper IUDs can even be used as a form of emergency contraception, as long as they’re placed within five days of having unprotected sex.
IUD removal
IUDs aren’t absorbed by the uterus when they expire (or when a woman no longer wants it), so they must be removed. And, as with insertion, the removal has to be done by a doctor. It’s a simple process: the doctor simply tugs on the strings and the T sides fold up, allowing for easy (and pretty pain-free) removal.
IUD cost
As of right now, IUDs are included in Obamacare’s free birth control requirement. However, for women without insurance — or eventually, for those who work for employers who don’t cover it — can pay anywhere from $150 to $1,000 for an IUD, though organizations like Planned Parenthood often provide low- or no-cost IUDs for women who need them.